BGI State of Colorectal Cancer Awareness Report Reveals General Awareness Gaps and Affordability Concerns.
To uncover attitudes and the biggest challenges facing colorectal cancer (CRC) awareness and screening, BGI Genomics today released its State of Colorectal Cancer Awareness Report, marking the first-ever global survey report on the world’s third most common cancer. This report is released on World Health Day, April 07, 2023, in line with achieving Health For All, and seeks to motivate action to tackle the health challenges of today and tomorrow.
This inaugural report seeks to better understand the global state of CRC awareness, as well as attitudes and actions towards CRC screening for average risk groups and CRC screening for hereditary genetic risk groups. 1,817 respondents from six countries and regions were surveyed: the U.K. (Western Europe), Hungary (Eastern Europe), Saudi Arabia (Middle East and Africa), Thailand (Southeast Asia), the Chinese mainland, and Hong Kong (North Asia).
Hungary had the highest global incidence rate of colorectal cancer, with 9,793 cases in 2020 based on World Cancer Research Fund data. CRC screening participation rate is very low in Hungary, so CRC is most commonly recognized at a late stage where there are fewer treatment options available.
Despite 51.5% reporting that there is insufficient information about CRC and 34.5% citing costs holding them back from CRC screening, the report reveals several optimistic findings. For example, 88.8% are more willing to go for screening upon learning about the 5-year survival rate of 90% for early CRC detection.
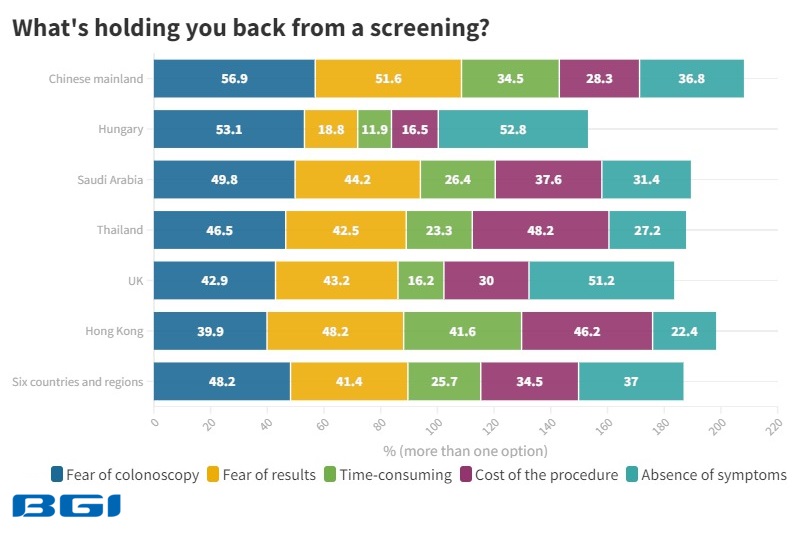
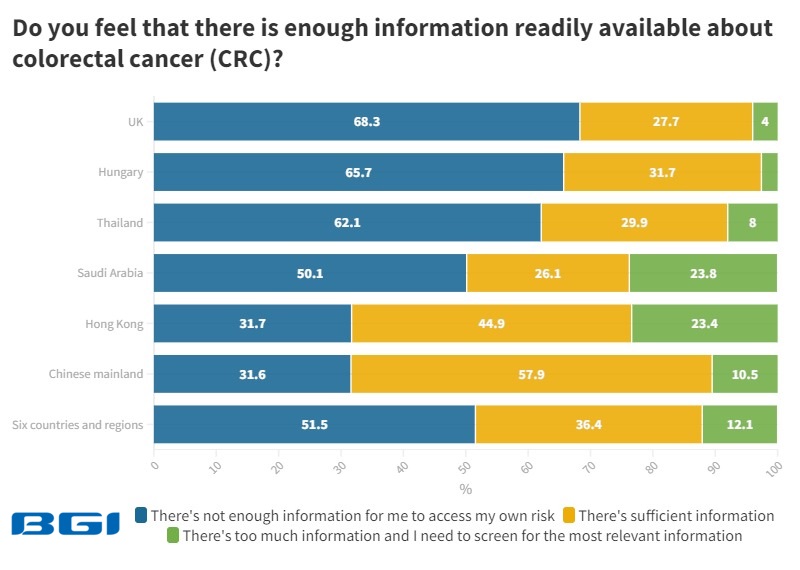
“Early CRC detection offers the best outcome for individuals and healthcare policy. The treatment cost of late-stage CRC is sometimes more than ten times higher relative to early-stage CRC but with far lower survival rates,” said Yantao Li, PhD, BGI Genomics Director of Colorectal Cancer Screening Programme, South-East Asia. “That’s why more countries or regions are promoting early screening programs. For example, the European Commission is ramping up CRC screening programs.”
Other key takeaways from the report include:
Colonoscopy is the best-known screening test, but there is scope to enhance the awareness of other tests such as fecal tests. Though colonoscopy (68.2%) is the best-known screening test, it is more expensive and cumbersome relative to fecal testing which is lesser known at 49.5%. To promote this more affordable and flexible option, fecal testing awareness
needs to be enhanced.
Doctors are the biggest factor for respondents to go for screening in the absence of symptoms. 62.5% will heed their doctor’s advice to undergo CRC screening. Therefore, it is vital that doctors are made more aware of CRC symptoms, ask the right questions to identify potential hereditary genetic risks, and offer patients a range of screening options, to fit different lifestyles and budgets. In our opinion, the best colorectal cancer screening test is the one a patient will do.
Respondents are split when asked about bringing their family members for screening. 55.7% are aware that a family history of CRC increases their risk. According to the National Comprehensive Cancer Network (NCCN) guidelines, these family members should start screening at age 40 or 10 years before the earliest diagnosis of CRC in the family. The good news is that 67.2% who had CRC or a family history of CRC have taken their family members for screening. Conversely, only 31.2% of all respondents have taken their family members for CRC screening.
As we wrote before, 5,000 Hungarians die of this disease every year: don’t forget to get tested!




